Background
Aphthous stomatitis, also known as recurrent aphthous ulcers or canker sores, is among the most common oral mucosal lesion physicians and dentists observe. Aphthous stomatitis is a disorder of unknown etiology that may cause significant morbidity. One or several discrete, shallow, painful ulcers are visible on the unattached oral mucous membranes. Individual ulcers typically last 7-10 days and heal without scarring. Larger ulcers may last several weeks to months and can scar when healing.
Pathophysiology
Although the process in idiopathic recurrent aphthous ulcers is usually self-limiting, in some individuals, ulcer activity can be almost continuous. Similar ulcers can be noted in the genital region. Behçet syndrome, systemic lupus erythematosus, and inflammatory bowel disease are systemic diseases associated with oral recurrent aphthous ulcers. Recurrent aphthous ulcers occur on nonkeratinized or poorly keratinized surfaces of the mucosa such as following:
- Labial and bucca mucosa
- Maxillary and mandibular sulci
- Unattached gingiva
- Soft palate tonsillar fauces
- Floor of the mouth
- Ventral surface of the tongue
- Inferior lateral surface of the tongue
The clinical presentation of aphthous ulcers is defined by the number of recurrences and severity of disease. Clinically, the number and size of the ulcers are the two main criteria used to divide ulcers into three forms: minor, major, and herpetiform. Simple aphthae are common and considered mild, with 1-4 episodes per year. In general, there are few lesions of the minor orherpetiform form. In contrast, complex aphthosis has a severe clinical course, with an almost continuous presence of minor or major ulcers. These may be debilitating and may also involve the genitalia of both men and women. It is imperative that these patients be evaluated to rule out Behçet disease as well as inflammatory bowel disease.
Recurrent aphthous ulcer minor (Mikulicz ulcer)
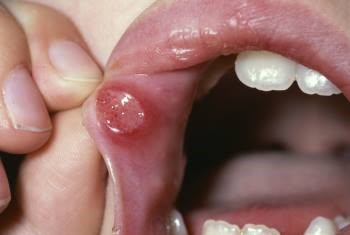
This is the most common form, accounting for 80-85% of cases. Discrete, painful, shallow, recurrent ulcers smaller than 1 cm in diameter characterize this form, shown in the image below. At any time, one or multiple ulcers can be manifest. These ulcers heal within 7-14 days without scarring. The periodicity varies among individuals, with some having long ulcer-free episodes and some never being free from ulcers..
Recurrent aphthous ulcer major (Sutton ulcer, periadenitis mucosa necrotica recurrens)
This form accounts for about 5-10% of cases and present as round or oval ulcers that range in size from 2-3 cm in diameter, as shown in the image below. Major aphthae typically present as a single ulcer, but multiple ulcers may occur. The ulcers present on the soft palate, lips, or oropharynx.
They may be deep with smooth or irregular borders. The ulcers may coalesce. Healing, which may take 6 weeks or even months, results in scarring; severe distortion of oral and pharyngeal mucosa may occur. These are more common in patients with HIV disease.
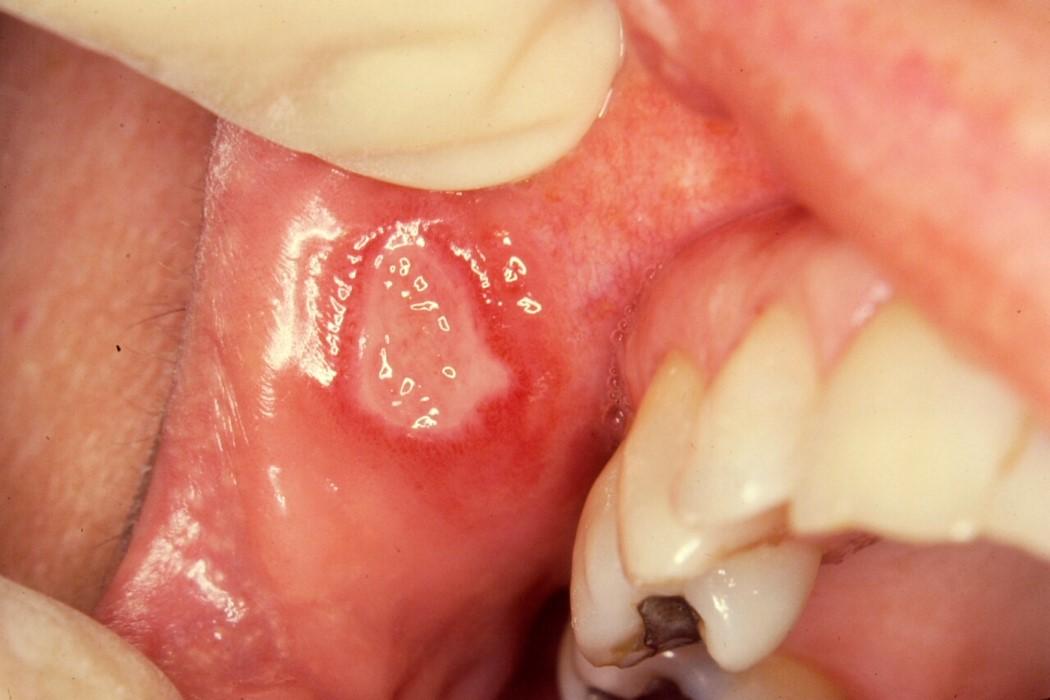
Major aphthous ulcer: Large oval ulcer with white pseudomembrane and raised red border located on the right upper labial mucosa adjacent to the buccal commissure. Note the irregular margin so typical in major aphthae.
Herpetiform recurrent aphthous ulcer
In this rare form (<5% of cases), ulcers are typically about 1-2 mm in diameter. The aphthae tend to occur in clusters or crops consisting of 10-100 ulcers. Clusters may be small and localized, or they may be distributed throughout the soft mucosa of the oral cavity. These too occur predominantly on unkeratinized mucosa, as shown in the image below. It is important to differentiate these ulcers from herpes simplex virus (HSV), which also may appear as recurrent crops. HSV is an infectious disease that often presents with vesicles that quickly ulcerate and involve the keratinized mucosa of the hard palate, dorsal tongue and attached gingiva.
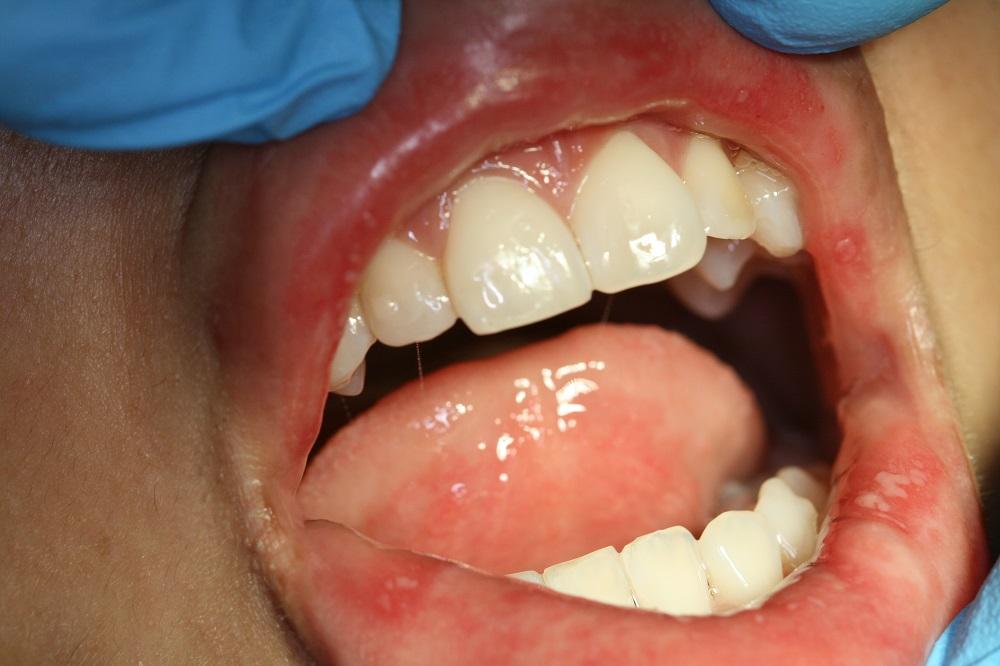
Herpetiform aphthous ulcer: Grouped and single tiny white to yellow ulcers scattered on the labial mucosa and on the ventral aspect of the tongue.
US frequency
Epidemiology
Recurrent aphthous ulcers are the most common oral mucosal disease in North America. They affect 20% of the population, with the incidence rising to more than 50% in certain groups of students in professional schools. Children from high socioeconomic groups may be affected more than those from low socioeconomic groups. [1] Note the following point prevalence and lifetime prevalence rates [2] :
- Point prevalence in the pediatric population in the United States: 1.2- 1.5%
- Lifetime prevalence in the pediatric population in the United States: 40.18%
International frequency
Recurrent aphthous ulcers occur worldwide and are reported on every populated continent. Recurrent aphthous ulcers affect 2-66% of the international population. [3] . Epidemiologic studies have been conducted in various subpopulations and report data on both point prevalence and lifetime prevalence, as follows:
- Lifetime prevalence in the adult population in the United States and Canada: 46.4-69.4%
- Europe lifetime prevalence: 36-37% [
- Sweden point prevalence: 0.5-2%
- Turkey point prevalence: 1.2-2.3
- Jordan lifetime prevalence: 78%
- Iran lifetime prevalence: 25.2%
- Sulaimani City, Iraq lifetime prevalence: 28.2%
- India point prevalence: 1.5% in Northern India
- India lifetime prevalence: 50.3%
Sex
In children and in some adult communities who are affected, the incidence of recurrent aphthous ulcer is higher in women and girls than in men or boys.
Age
Recurrent aphthous ulcer minor is the most common form of childhood recurrent aphthous ulcer. Approximately 1% of American children may have recurrent aphthous ulcers, with onset before age 5 years. The percentage of patients who are affected decreases after the third decade.
Recurrent aphthous ulcer major has a typical onset after puberty and can persist for the remainder of an individual’s life, although after late adulthood episodes become much less common.
Herpetiform recurrent aphthous ulcer first occurs in the second decade of life; the majority of persons have onset when younger than 30 years. The frequency and the severity of episodes may increase during the third and fourth decades and then decrease with advancing age.
Author: Ginat W Mirowski, MD, DMD; Chief Editor: William D James
Top ,.. top top … post! Keep the good work on !
Itís difficult to find educated people about this subject, but you sound like you know what youíre talking about! Thanks
I¦ve been exploring for a little bit for any high-quality articles or weblog posts on this kind of house . Exploring in Yahoo I eventually stumbled upon this website. Studying this info So i¦m glad to convey that I have a very excellent uncanny feeling I came upon exactly what I needed. I so much for sure will make sure to don¦t fail to remember this web site and provides it a look on a relentless basis.
Thank you
Loving the info on this site, you have done great job on the articles.
Hello.This post was really fascinating, particularly because I was searching for thoughts on this topic last couple of days.
I couldn’t resist commenting
Very interesting info !Perfect just what I was searching for!